Brien Center Talk Highlights Mental Health Effects of COVID

PITTSFIELD, Mass. — The COVID-19 pandemic had immediate and lasting effects on mental health and on providers.
During a community conversation titled "The Impact of the Pandemic on Mental Health and How to Manage Moving Forward," professionals from the Brien Center highlighted ways to heal from the stress and trauma of a global pandemic.
The organization provides a wide array of services ranging from behavioral health and emergency services to family mental health and substances abuse disorders. It works with community programs and offers personal counseling and residential treatment.
Its work was disrupted at the very start of the pandemic, forcing its medical professionals, therapists and clinicians to revamp how to deliver services during the crisis.
"I can tell you that when I started in my role, I never thought that I would have to manage or figure out how to successfully manage a pandemic and still provide services but we did that," CEO Christine Macbeth said.
"And a matter of fact, for 100 years we have been providing face-to-face services and when I say weeks, I literally mean weeks that we very quickly moved to a telehealth model of care, if you will. We invested significantly in upgrading our IT system, bought new laptops and phones so our clinicians could keep virtual appointments with their clients. However, that said, remember we still have residential programs and we had well over 100 people living in our residential programs at the time and we still do and our residential staff is nothing less than heroic during that period."
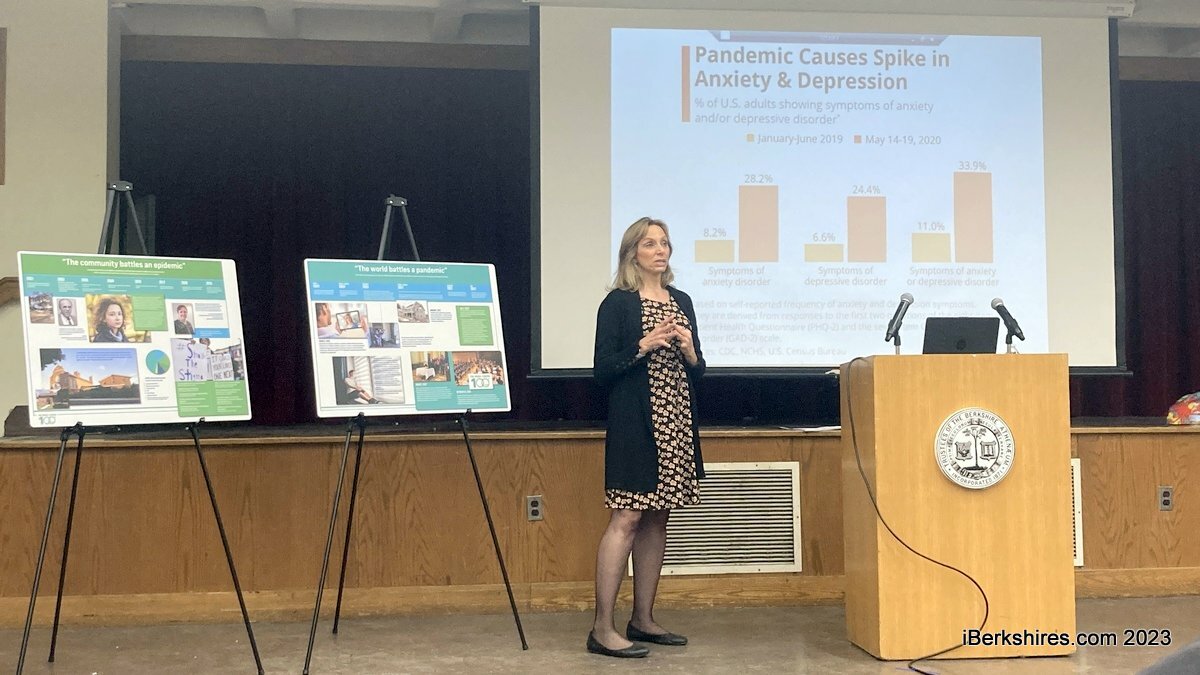
From January through June 2019, 11 percent of adults in the United States reported symptoms of anxiety and depression. That number skyrocketed to nearly 34 percent as the pandemic took hold in May 2020.
Similarly, the U.S. Centers for Disease Control data showed that 37 percent of youth experienced poor mental health during COVID-19 and 44 percent experienced persistent feelings of sadness or hopelessness in the past 12 months.
Macbeth pointed out that there has been a dramatic increase in the need for mental health services in the last three years and that, finally, state officials have begun to recognize the "significant, chronic underfunding" for community-based behavioral health providers.
During the pandemic, 20 percent of health-care workers left the field because of a mixture of occupational stress and pay.
Medical Director Dr. Jennifer Michaels said the community and the health care system also needs to be healed.
"Twenty percent of our staff at the Brien Center are no longer there. We lost most of our therapists and yet we're supposed to do the same work, even more, with less staff," she said.
"So we need more staff and to attract more staff, we need to pay them well so they want to work, and we need to also create programs like advocacy, loan forgiveness for doing this kind of work is imperative. Right now, a nurse working at the Brien Center could make a third as much as somebody who is a traveling nurse or working in a union or a different group somewhere else."
Last week, the World Health Organization ended the emergency status for COVID-19 and, on Thursday, masks were no longer required at Berkshire Health Systems' facilities. Also last week, Surgeon General Dr. Vivek Murthy released an advisory calling on the public health crisis of loneliness, isolation, and lack of connection in our country.
"The physical health consequences of poor or insufficient connection include a 29 percent increased risk of heart disease, a 32 percent increased risk of stroke, and a 50 percent increased risk of developing dementia for older adults. Additionally, lacking social connection increases risk of premature death by more than 60 percent," it reads.
Michaels explained that loneliness is so toxic because humans are social animals and release oxytocin, or the "love hormone," when around others.
"About a third of Americans reported serious loneliness during COVID and more than half of Americans feel lonely at any given time," she reported. "So this is like an opportunity. This isn't just the end of the story. This is hopefully the beginning of the story."
She highlighted the importance of good social connections for longevity and urged audience members to examine their relationships.
Michaels also spoke to the pandemic's production of "toxic stress" and its dangers. She explained that a stressed-out brain feels like it is constantly under attack, often overestimating threats, underestimating opportunities, and narrowing one's world.
"And the other thing is you miss out on all the fun," she said.
"So this is the experience of some people who are recovering from COVID. Their brains are still in alarm mode even though you know the emergency is supposedly really over and we're here tonight and we're feeling pretty safe."
Without minimizing the importance of medication, the medical director offered suggestions for creating a positive brain that include making a gratitude list, walking, meditating, connecting with others, and playing games.
The Brien Center offers a variety of treatment programs and recently launched a Community Behavioral Health Center to offer same-day services to MassHealth clients.
During the event, Michaels conducted mindful breathing exercises in which attendees were asked to count the number of breaths they took in one minute. For some, this was a stark realization that they need to take a deep breath.
Additional talks will be held throughout Berkshire County beginning at 5:30 p.m. on
- May 24 at the Lenox Library
- May 31 at the North Adams Public Library
- June 7 at Berkshire South Regional Community Center
Tags: mental health,
















